Ambulatory Blood Pressure Monitoring: A Thorough Approach to the Diagnosis & Treatment of Uncontrolled Hypertension
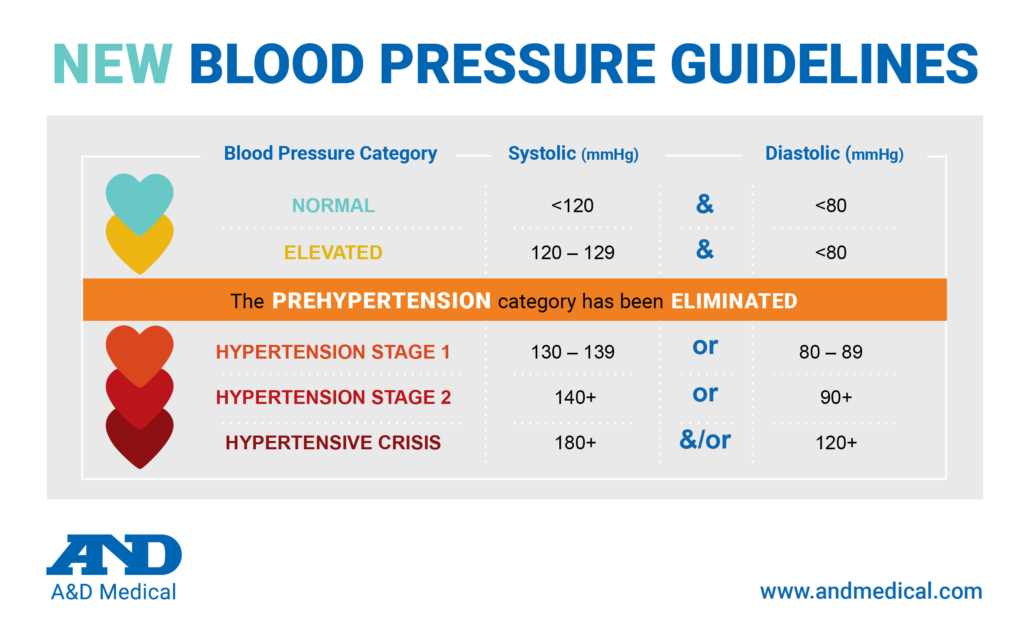
Known as the “silent killer”, uncontrolled hypertension is the leading cause of heart disease, stroke and death in the United States1. Due to the prevalence of the disease, among other reasons, the American Heart Association (AHA) and American College of Cardiology (ACC) changed their blood pressure classifications to help raise awareness and begin the diagnosis and treatment of heart disease before it becomes as severe.
The early diagnosis of hypertension alone, however, is not enough to curb the issue. Healthcare providers must work effectively with their patients to control hypertension through proven methods, such as medication and lifestyle changes, to stall or eliminate the prognosis of heart disease and death.
In cases of undiagnosed and/or uncontrolled hypertension, the increased utilization of 24-hour Ambulatory Blood Pressure Monitoring (ABPM) can be a crucial step towards better diagnosis and management of hypertension.
The disease state of hypertension is so prevalent that it now affects over 100 million Americans, nearly 1/2 of the country’s population2. Of these, only approximately 53% are controlled3, leaving nearly 40% of hypertensive Americans either undiagnosed or uncontrolled. To address the growing health risk, in 2017, the ACC and the AHA both updated the blood pressure (BP) guidelines, lowering thresholds to implement earlier interventions at a BP of 120/80 or higher4.
As a controllable condition, accurate diagnosis and management of hypertension is critical because it offers great potential to prevent heart attacks and strokes, and it can save patients and providers costs associated with myriad cardiovascular diseases. In fact, the ACC, the AHA4, and The Million Hearts 2022 initiative prioritized accurately identifying hypertension as the first step in the goal preventing 1 million heart attacks5, realistically reducing cardiovascular events by 30%, and all causes of mortality by 25%4.